More importantly, they will keep you informed about your baby's current state of health and what to expect in the coming days. 
Medical staff will first focus on getting your baby into a stable condition and then they will seek to find answers to the questions that will be weighing on your mind, like what has caused your baby’s low score.Īs medical staff works to discover if there is an underlying condition or another cause of your baby's low score, they will keep you updated throughout the process. What Happens If My Baby Has A Low APGAR Score? To get the overall score for an infant, a score of 0 to 2 will be assigned for each of the 5 categories.ġ means there are fewer than 100 beats per minute (not very responsive)Ģ means there are more than 100 beats per minute (baby is vigorous)Ġ means no response to their airways being stimulatedġ means there is a grimace during stimulationĢ means there is a grimace and cough/sneeze during stimulationĠ means the baby's entire body is blue/paleġ means the baby has good color except on their hands/feet (acrocyanosis)Ģ means the baby is completely pink and has good color A score under 4 means that prompt, life-saving resuscitation measures are necessary. 
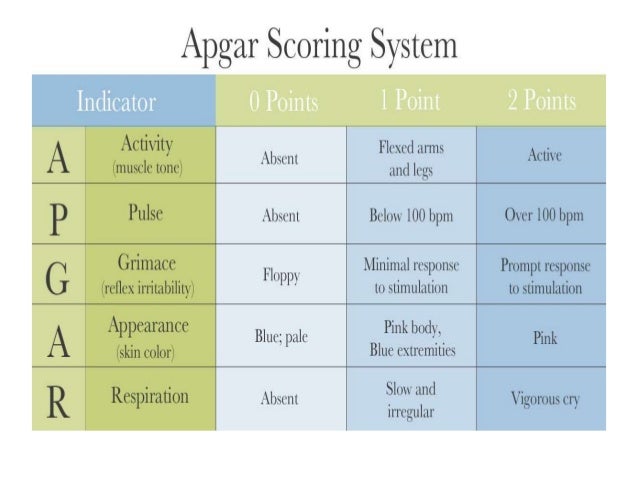
A score between 4 and 6 indicates that breathing assistance may be required. R stands for Respiration (breathing rate, effort, and pattern)Ī score between 7 and 10 is considered normal. G stands for Grimace response (reflexes and crying)Ī stands for Activity (muscle tone and flexion) P stands for Pulse (heart rate or beats per minute) Your baby will continue to be scored in five-minute increments until he achieves a 7 or higher.Ī stands for Appearance (skin color, pink or blue) Every baby is scored at one minute of life and then again at five. In short, it is a baby's first assessment. Generally speaking, the “APGAR Scoring System” is a method to quickly summarize the health of a newborn. The most routinely used measure of health status of newborns is the Apgar score, typically quantified at 1, 5, and 10 minutes after birth.1 Our recent population based studies have shown that non-malformed term infants born with lower Apgar scores within the normal range (7 to 9) at 1, 5, or 10 minutes are at higher risk of adverse long term outcomes, such as epilepsy, cerebral. The test is performed one minute after your baby’s birth to see how well your baby coped with the birth process and again at five minutes to see how well your baby is adjusting to their new environment. Keep in mind that most babies RARELY get a perfect score. An Apgar score is a simple way for doctors or midwives to quickly assess the health of a newborn. Every baby gets an APGAR score, but as a parent, it can be a completely foreign topic that leaves you worried and confused, especially if your infant ends up getting a low score. Your baby’s score is very important because it will determine their medical care during their first few days at the hospital. Apgar score is usually done to the baby twice: once at one minute after birth and again at 5 minutes after birth. However, several possible causes of low Apgar scores exist, such as perinatal asphyxia and congenital infections 69. if Apgar = RR then Resuscitation must = 2-6 or 8.The APGAR test is a standard procedure that is administered for every infant. A total score of 7-10 is considered normal, and a lower Apgar score indicates depressed vitality. Apgar score is cross-checked with Resuscitation e.g. Apgar score is cross-checked with Condition on Discharge and MUST ONLY be present if Condition on Discharge = 3. In singleton pregnancies only the first field should be completed. Provision is made for coding the Apgar score of three babies. If the baby is receiving active resuscitation (intubation) the Apgar score is probably not valid and the boxes should be infilled with RR. For liveborn babies who just live for one or two minutes a score should be entered it may be 00 or 01. For stillborn babies the field should be left blank. The Apgar score is the common scoring method of the babys well being after the birth, and is based on a combination of the heartbeat, respiration, skin colour, muscle tone and movement. It is named after Dr Virginia Apgar, who developed the score in 1952, she was a Professor of Anesthesiology at Columbia University in the USA, she died in 1974 3). Recording Rules The appropriate code should be entered for a live birth as follows: NR not recorded 00-10 actual Apgar score at 5 minutes (or death before 5 minutes) RR Baby being actively resuscitated at the 5 minute check (therefore Apgar score cannot be accurately taken) Points to Note 1. The Apgar score guides midwives, doctors and nurses as to whether a baby needs immediate treatment or monitoring. mandatory implementation date 01/10/10 Definition A score based on assessment of 5 variables in the baby, each rated from 0-2 (0 worst, 2 best). Data Change Notice: 1008/06 (Fast track) Changes to SMR Data Manual: Changes requested as a result of the SMR02 Quality Assurance Report - Published April 2010.
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |

 RSS Feed
RSS Feed
